Case Study An Elderly Man With Slurred Speech and Left Side Weakness
Case Study An Elderly Man With Slurred Speech and Left Side Weakness
A 60-year-old man is brought to the ER by ambulance because of slurred speech and left side weakness. His wife states they went to bed at 11pm and woke up at 5am when she noticed his symptoms. He is right handed with a history of coronary artery disease, hypertension, and hypercholesterolemia and a heart attack at age 50. He currently is unable to move his left arm and leg.
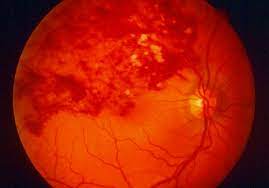
He had an episode of amaurosis fugux (blindness)in his right eye one month ago that lasted for 5 minutes. Around 3 months ago his wife states he had bilateral pain in his legs while they were on a walk that lasted about 15 minutes. He is taking a baby aspirin a day an ACE inhibitor, and statin as well. He does have a history of alcohol use and smoking in the past but stopped after his heart attack.
His blood pressure is 195/118 Pulse 106, Respiratory rate 18, Temperature 99.8, o2 sat is 97% on room air. Although his pupils are equal and reactive, and the ocular movements are intact, he is unable to turn his eyes voluntarily toward the left side.
The neck is supple, there is no jugular vein distension, and there are no bruits. The lungs are clear heart sounds regular without murmurs, and abdomen is normal. The limbs are not well perfused distally. The neurologic examination reveals that he is alert and oriented, although he does not recognize he is sick. He shows loss of awareness and attention with respect to objects or stimuli on his left sides.
He has mild dysarthria but, his speech is fluent, and he understands and follows commands very well. There is mild weakness on the left side of the face and left sided homonymous hemaianopsia, but there is no nystagmus or ptosis, and no tongue or uvula deviation. He is not able to move his left arm and leg, has hyperreflexia, and the left great toe is upgoing.
- What are two questions you would ask this patient?
- Identify the subjective data for this patient.
- Identify the objective data for this patient.
- What is the likely diagnosis?
Your response should include evidence of review of the course material, websites, and literature through proper citations using APA format.
Case Study 2 Overview
Mr. Hall, a 65-year-old male patient is admitted to the ICU through the ER with right-sided weakness and slurred speech. He has a hypertension & type 2 diabetes. He also reports a long history of smoking at least a pack of cigarettes each day. The CT scan from shows an intracranial hemorrhage.
In this discussion:
1. What is the most likely cause of the hemorrhagic stroke?
2. Describe the risk factors for both hemorrhagic & ischemic stroke.
3. Discuss the most likely area of the brain affected by the stroke.
4. Discuss this patient’s short and long-term plan of care & prognosis.
Include citations from the text, the Shadow Health simulation assignment, and/or the external literature in your discussion posts
Remember to respond to at least two of your peers. Please refer to the Course Syllabus for Participation Guidelines & Gradin Criteria
Case Study 2: Mr. Hall Sample Solution
The case study concerns Mr. Hall, a 65-year-old male who was moved from the emergency room (ER) to the intensive care unit (ICU) with right-sided weakness and slurred speech. He is a known hypertensive patient, has type 2 diabetes mellitus, and long-standing history of tobacco use. The CT scan investigation revealed intracranial hemorrhage.
Cause of his Stroke
Mr. Hall has a hemorrhagic stroke that could be from different causes. However, his hypertension is the most likely cause of his hemorrhagic stroke. Persistently high blood pressure can rupture the small vasculature of the brain leading to a hemorrhage that occupies space in the fixed skull space to cause the focal symptom Case Study: An Elderly Man With Slurred Speech and Left Side Weakness. Paradoxically, hypertension treatment can also lead to ischemic stroke when the management is overzealous enough to reduce the blood pressure to levels causing hypoperfusion. This phenomenon is rare but occurs more in elderly patients.
Risk Factors for Stroke
Both hemorrhagic and ischemic stroke can be caused by hypertension, among other risk factors. The most common risk factors for hemorrhagic stroke include but are not limited to poorly controlled hypertension (Kuriakose & Xiao, 2020), coagulopathies with bleeding tendencies, vascular malformations, and angiopathies Case Study: An Elderly Man With Slurred Speech and Left Side Weakness. These causes increase the risk of bleeding in the brain leading to stroke. The bleeding can be acute or long-standing, depending on the cause.
Ischemic stroke common risk factors include but are not limited to familial predisposition, hypertension, cardiac disease including atrial fibrillation, hyperlipidemia, diabetes mellitus, alcohol use, and smoking (Kuriakose & Xiao, 2020). These causes increase the risk of reduction or occlusion of blood supply to certain brain regions leading to ischemic stroke Case Study: An Elderly Man With Slurred Speech and Left Side Weakness. Mr. Hall has three risks for ischemic stroke and only two for hemorrhagic stroke: smoking, diabetes mellitus, and hypertension a long history of smoking and hypertension and smoking for hemorrhagic stroke.
Brain Areas Affected By Stroke
Stroke can affect many areas of the brain, but the major areas include but are not limited to the frontal lobe, parietal lobes, basal ganglia, and brain stem. However, the area affected is determined by the artery affected by ischemia or hemorrhage. The most common vessel is the middle cerebral artery (Hui et al., 2021), making the frontal lobe, temporal lobe, basal ganglia, and internal capsule the most common areas in cases of infarction.
Cerebellar stroke is also not uncommon. Mr. Hall has slurred speech and right-sided weakness, suggesting that the left temporal lobe was the most likely affected area of the brain. The Wernicke’s area is located in the temporal cortex and is responsible for speech-motor coordination. Notably, Wernicke’s area is not the only area in the speech pathway.
Mr. Hall’s Management and Prognosis
The management goals for Mr. Hall are promoting repairs and preventing the deterioration of his status. In the short term, blood pressure reduction and prevention of pressure symptoms, including seizures, are prioritized Case Study: An Elderly Man With Slurred Speech and Left Side Weakness. Therefore, antihypertension medications, anticonvulsants, and diuretics to relieve intracranial pressure would be used (Wajngarten & Silva, 2019).
Thrombolysis may worsen the bleeding. In the long term, the aim is to help Mr. Hall regain his cognitive, motor, and speech function will be important. Physiotherapy, speech therapy, and occupational therapy will be offered to improve his prognosis. Risk prevention will include hypertension management, teaching on smoking cessation, and regular sugar controls for Mr. Hall.
Conclusion
Mr. Hall had a hemorrhagic stroke, most likely in the left temporal cortex. The known risk factors for his stroke are hypertension and longstanding smoking. His shirt term management will include the use of antihypertensives, anticonvulsants, and diuretics Case Study: An Elderly Man With Slurred Speech and Left Side Weakness. However, the long-term will be rehabilitative and restorative. Physical, speech and occupational therapies will be prescribed. Prevention of his risk factors will also be prioritized for a better long-term prognosis.
Case Study An Elderly Man With Slurred Speech and Left Side Weakness References
- Hui, C., Tadi, P., & Patti, L. (2021). Ischemic Stroke. In StatPearls [Internet]. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK499997/
- Kuriakose, D., & Xiao, Z. (2020). Pathophysiology and treatment of stroke: Present status and future perspectives. International Journal of Molecular Sciences, 21(20). https://doi.org/10.3390/ijms21207609
- Wajngarten, M., & Silva, G. S. (2019). Hypertension and stroke: Update on treatment. European Cardiology, 14(2), 111–115. https://doi.org/10.15420/ecr.2019.11.1
Ischemic Heart Disease Discussion Sample Paper
Question One
The risk factors present in this case include advanced age (58 years), male gender, and elevated blood pressure 122/74. Male gender and advanced age the non-modifiable risk factors for angina (Kloner & Chaitman, 2017) while elevated blood pressure is modifiable. However, if not checked, Bill’s blood pressure may progress to hypertension which could be fatal.
Question Two
The goals for treatment include increasing oxygen supply to the heart and reducing the oxygen demands of the myocardium (Kloner & Chaitman, 2017). Pains due to angina occur when the oxygen demands exceed supply. An approach to reduce heart rate, preload, and afterload and improve coronary blood flow would relieve the symptoms.
Question Three
I recommend an organic nitrate like nitroglycerin to Bill to prevent the occurrence of angina attacks. Nitroglycerin is a vasodilator (Soman & Vijayaraghavan 2017) that works by dilating the coronary blood vessels leading to an increase in blood supply to the heart.
Question Four
For acute episodes of angina, aspirin, clopidogrel or heparin would be effective. The drugs are anticoagulants. They prevent clot formation in coronary blood vessels improving blood flow to the heart. Due to increased heart perfusion, there will be decreased pains.
Question Five
Beta-blockers decrease cardiovascular mortality since they reduce the chances of myocardial infarction and are beneficial when cardiac infarction has not occurred (Kloner & Chaitman, 2017). I will recommend them for additional medical outcomes. They include atenolol and metoprolol.
Question Six
The drug therapy monitoring plan in the case of Bill would aim at determining the possible toxicity of the medications and whether the problem resolves. The drug therapy monitoring will take place after every 24 hours for two weeks. Optimal therapy improves angina symptoms within two weeks. The monitoring will include measuring the blood pressure, checking for signs of dizziness, headache, peripheral edema, and constipation when calcium channel blockers are used. A report on pain resolution would be necessary to determine the effectiveness of the medications.
Question Seven
Patient education includes explaining the causes of angina, the diagnosis, and prevention measures. The approach would include advising Bill on the importance of physical activity, not smoking, and the importance of screening for diabetes and hypertension regularly. Drug adherence and the ways to take them would also be part of the plan.
References
- Kloner, R., & Chaitman, B. (2017). Angina and Its Management. Journal Of Cardiovascular Pharmacology And Therapeutics, 22(3), 199-209. https://doi.org/10.1177/1074248416679733
- Soman, B., & Vijayaraghavan, G. (2017). The role of organic nitrates in the optimal medical management of angina. E-Journal of Cardiology Practice, 15(2). https://www.escardio.org/Journals/E-Journal-of-Cardiology-Practice/Volume-15
